
IVF NewsNews: ART & Embryology training program
Chennai Fertility Center and Research Institute 03 October 2023

The International School of Embryology was established to offer training for clinicians in Advanced Reproductive Technologies. Our skill and precision to all aspirants help them to know in-depth knowledge and experience. The members of our teaching faculty aim to bring doctors and embryologists to the highest level of knowledge about Reproductive Techniques and practical capability in the field. Our courses cover basics in Andrology, embryology, ICSI, and cryosciences (Hands-on). Training Batch Schedule:
# November 2023 - 15th to 29th November
Limited Seats. For admission Contact 9003111598 / 8428278218 (Whats app) [ Full Article ] Webinar: NAVIGATING INTERNATIONAL SURROGACY
International IVF Initiative 01 October 2023
Tuesday, 3rd October (3 pm EDT / 8 pm UK / 9 pm CET) Moderators: Presenting: [ Full Article ] I3 Revisited: How Green is Your IVF?
International IVF Initiative 01 October 2023

This video is one of many educational resources produced by the International IVF Initiative (I3). As a worldwide movement, I3 focuses on improving education and refining methods in assisted reproductive technologies. To explore a wider range of educational content, we invite you to visit https://ivfmeeting.com.
Roisin is an embryologist with CRGW where she is currently working towards registration with the HCPC. She completed her Masters at Trinity College Dublin before starting her career in the field in 2016 (?) with the Merrion Fertility Clinic in Dublin. She proceeded to gain experience in andrology at a variety of clinics and the European Sperm Bank before starting with CRGW in 2021. She has a particular interest in Male factor infertility, fertility preservation and sustainability within the IVF clinic. [ Full Article ] Webinar: TRACE ELEMENTS
International IVF Initiative 12 September 2023
Tuesday, 19th September (3 pm EDT / 8 pm UK / 9 pm CET) [ Full Article ] News: Human Embryo-Like Models Created from Stem Cells
IVF.net Newsdesk 12 September 2023
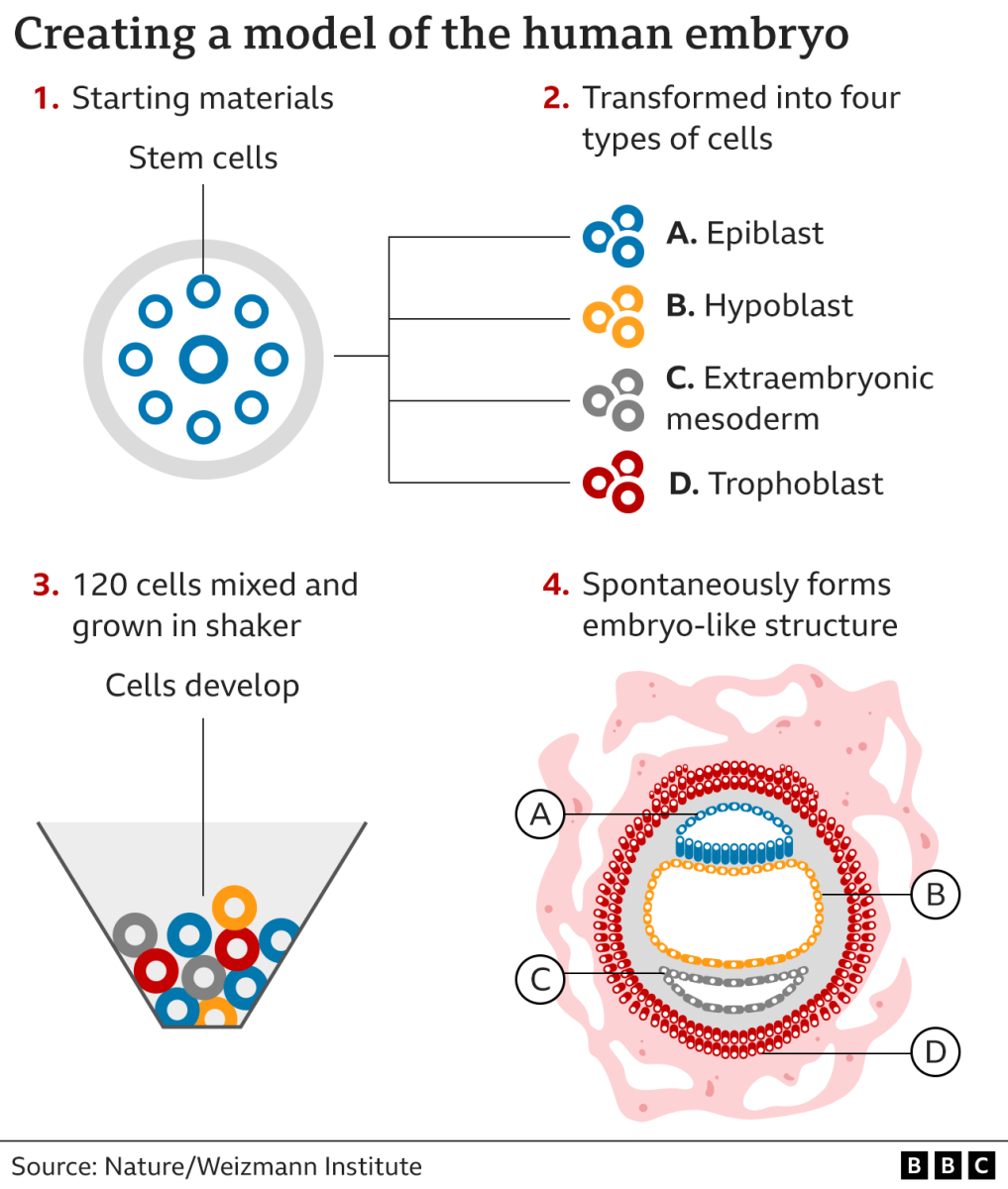
The challenge of studying human development shortly after implantation has been restricted due to the ethical and technical difficulties connected with in-utero growth post-implantation. Yet, recent breakthroughs have been made using mouse naïve embryonic stem cells (ESCs) to develop embryo-like structures. Extending this method, scientists have now successfully developed complete human embryo models using unmodified human naïve ESCs. These models mimic almost all the known features of post-implantation human embryos up to 14 days after fertilization. In a revolutionary step, researchers at the Weizmann Institute have cultivated an entity resembling a 14-day-old human embryo using stem cells, without resorting to sperm, eggs, or a womb. Remarkably, this "embryo model" exuded hormones that registered a positive result on a pregnancy test in a laboratory setting. These embryo models offer a promising and ethically sound method to probe into the earliest phases of human existence. The transition from a vague cluster of cells post-fertilization to a recognizable entity during a prenatal scan undergoes significant transformations, which, unfortunately, are inadequately understood despite being vital as it's a period that often results in miscarriages or birth defects. The novelty of this research, shared in the Nature journal, lies in its comprehensive replication of primary structures seen in early embryos. This achievement, creating a vivid representation of a 14-day-old human embryo, is unprecedented. Initiating with naïve stem cells, which can morph into any body tissue, they used chemicals to guide the cells into four primary types present during an embryo's earliest stages. Astonishingly, around 1% of these cultivated cells spontaneously organized into a structure reminiscent of a human embryo. Simply providing the right environment allows the cells to autonomously arrange themselves. These models matured until they resembled 14-day post-fertilization embryos, a significant juncture in numerous countries that often marks the limit for standard embryo studies. Through these models, scientists hope to elucidate cellular differentiation processes, observe initial organ formation stages, and gain insights into inherited or genetic conditions. Notably, the study indicates that certain embryo parts won't develop unless enclosed by early placenta cells. This research could even aid in enhancing IVF success rates. However, this method's present 99% failure rate demands refinement, points out Prof Robin Lovell Badge from the Francis Crick Institute, who otherwise praises the study. In conclusion, while these models showcase immense potential, using them for pregnancy remains firmly off the table, with ethical, legal, and practical reasons making it an impossibility.
Sources Weizmann Institute of Science Nature BBC News
[ Full Article ] News: ART & Embryology training program
Chennai Fertility Center and Research Institute 02 September 2023

The International School of Embryology was established to offer training for clinicians in advanced reproductive technologies. Our skill and precision to all aspirants help them to know in-depth knowledge and experience. The members of our teaching faculty aim to bring doctors and embryologists to the highest level of knowledge about reproductive techniques and practical capability in the field. Our courses cover basics in Andrology, embryology, ICSI, and cryosciences (Hands-on). Training Batch Schedule# September 2023 - 4th to 18th September $ October 2023 - 03rd to 17th October # November 2023 - 15th to 29th November $ December 2023 - 04th to 18th December Limited Seats. For admission Contact 9003111598 / 8428278218 (Whats app) [ Full Article ] News: ART & Embryology training program
Chennai Fertility Center and Research Institute 02 September 2023

October 2023 Training Batch Schedule - 3rd October 2023 - 17th October 2023. The International School of Embryology a unit of Chennai Fertility Centre and Research Institute was established to offer training in Advanced Reproductive Techniques and Embryology for clinicians and embryologists. It will help them to know in-depth knowledge and have good hands-on training. The members of our teaching faculty aim to bring Clinician and Embryologists to the highest level of knowledge about Assisted Reproductive Technology and practical capability. Our courses cover basics in Andrology, embryology, ICSI, and cryosciences (Hands-on). Limited Seats. For admission Contact 9003111598 / 8428278218 (Whats app) [ Full Article ] News: ART & Embryology training program
Chennai Fertility Center and Research Institute 02 August 2023

September 2023 Training Batch Schedule - 4th September 2023 - 18th September 2023. The International School of Embryology was established to offer training for clinicians in advanced reproductive technologies. Our skill and precision to all aspirants help them to know in-depth knowledge and experience. The members of our teaching faculty aim to bring doctors and embryologists to the highest level of knowledge about reproductive techniques and practical capability in the field. Our courses cover basics in Andrology, embryology, ICSI, and cryosciences (Hands-on). Limited Seats. For admission Contact 9003111598 / 8428278218 (Whats app) [ Full Article ] Announcement: AI and IVF Survey
Giles Palmer 19 July 2023

Calling all Reproductive Biologists, Embryologists/Andrologists in ART labsIVF2.0 with the International IVF Initiative (I3) is conducting a survey about Artificial Intelligence. This survey will take approximately 10-15 minutes of your time. Awareness, Use and Understanding of AI in the ART LaboratoryThe aim of the survey is: A) Assess the level of awareness among ART laboratory professionals regarding the applications and potential benefits of AI technology. This survey is being managed by Community Research, an independent research agency that will collect and process different types of data from you. To participate, simply click on the button! Thank you in advance for your time and valuable contribution. Best regards, https://www.smartsurvey.co.uk/s/IVFAI20/ [ Full Article ] I3 Revisited: The Curious Case of Lactate, a Blastocyst and an Endometrium
Professor David Gardner 19 July 2023
Lactate is typically considered a “waste-product” of glucose metabolism, produced through glycolysis, when there is insufficient oxygen available. But why does the blastocyst produce significant quantities of lactate even when there is an abundance of oxygen? The answer to this question will make you rethink completely the significance of metabolic functions, and you will discover that this quirky metabolic trait is a prerequisite for a tissue that needs to invade, establish a blood supply and avoid immuno rejection. Spoiler alert – cancers use the same trick as our beautiful blastocysts to invade surrounding tissues! PROFESSOR DAVID K. GARDNER, FAA David is the Scientific Director of Melbourne IVF and a Distinguished Professor in the School of BioSciences, University of Melbourne. This video is one of many educational resources produced by the International IVF Initiative (I3). As a worldwide movement, I3 focuses on improving education and refining methods in assisted reproductive technologies. To explore a wider range of educational content, we invite you to visit https://ivfmeeting.com. [ Full Article ] |